

In Vitro Fertilization
Some couples require the specialized treatment of In vitro fertilization, in which the egg is fertilized outside of the body. IVF was first used successfully in 1978. It has since become a regular medical procedure resulting in thousands of births.
Step One: Ovarian Follicle Development
Women usually grow a single egg in a month. In order to maximize the number of eggs for in vitro fertilization, the patient takes medication that can be utilized alone or in combination to induce several follicles to develop. Egg development is monitored by ultrasound imaging of the ovaries and by monitoring of blood hormone levels. When the follicles reach a satisfactory size, you will receive an injection of human chronic gonadotropin (HCG) in the evening or early morning. This initiates the final phase of egg development in preparation for egg retrieval. The decision of when you receive the HCG is based on follicle size and the time that the retrieval will occur (usually 34-36 hours following the injection). We recommend limiting very strenuous activity and exercise during this phase, as the ovaries are maximally stimulated. Strenuous activity could result in rupture of the follicles or twisting of the ovaries. You will receive other pre-operative instructions at this time.
Step Two: Egg Harvesting – Oocyte Retrieval
Egg retrieval from your ovaries takes place between 34 to 36 hours after the HCG injection. This timing is critical. It is the time the egg matures, just before ovulation. The ultrasound guided aspiration is usually performed in the office with intravenous sedation. For the procedure, an IV is started in the arm and medication given to induce sedation, minimize discomfort and to prevent nausea. A needle is introduced through the vagina into the ovaries and the eggs are aspirated. The follicle aspiration sometimes causes mild discomfort. Antibiotics are given through the IV when retrieval is completed, then the IV is removed. The patient spends up to an hour in our recovery room, then may go home. The IV site and vein used may become tender and hardened. If there is concern, please notify the doctor. Following this procedure, you may have a small amount of spotting or bleeding, neither of which are serious. If there is increasing abdominal discomfort and/or fever, you should notify the office immediately. Complications to the bowel, blood vessels and bladder are rare with ultrasound-guided aspiration of eggs. Our patients undergo the egg harvesting procedure in our office under local anesthesia and IV sedation. Not only is this environment more comforting and convenient, there is the added benefit of not incurring hospital fees.
Step Three: Semen Collection
Your partner should refrain from ejaculation for two days prior to your intrauterine insemination or ART procedure. If you are undergoing egg retrieval, your partner will be requested to provide a semen specimen that he may either bring to the clinic immediately before the retrieval, or that he may collect by masturbation in a private area after the egg retrieval has been performed. Semen collection must be done under certain conditions; your partner will be given instructions for collection.
tep Four: In Vitro Fertilization Laboratory
Immediately after oocyte collection procedure, the follicular fluid containing the eggs is taken to the ART laboratory. The laboratory is equipped with advanced equipment for culture of the eggs and sperm. The eggs are placed in a petri dish in a special culture medium which consists of several essential chemicals. We retrieve as many eggs as possible and immediately transfer them to the incubator where conditions simulate body conditions as closely as possible (temperature, nutrients, sterility, etc.). The processed sperm is introduced into the medium containing the eggs for fertilization. Quality control and security measures are strictly monitored while eggs and sperm are in the ART laboratory. We recommend that all the eggs be inseminated so that there will be a chance of obtaining several embryos. If there is male factor infertility, this is the point at which we would perform ICSI to assure fertilization.
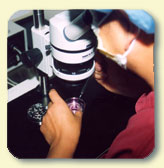
The embryos are examined daily. When Pre-implantation Genetic Diagnosis has been recomended, it is performed at this time. If fertilization and growth occur normally, you can return for embryo transfer on the second or third day after retrieval.
Step Five: Uterine Embryo Transfer
Transferring the embryo is done in the same area where the eggs are retrieved, however neither anesthesia nor intravenous sedation are required. The procedure is very similar to having a PAP smear. A speculum is placed into the vagina to view the cervix. The embryos are placed in a catheter (a tubular instrument) along with a small amount of fluid, and then the tiny plastic tube is introduced into the uterus through the cervix and the embryo(s) are transferred into the endometrial cavity. After this you will need to rest in bed for one hour with your head down and feet up. After going home, you need to rest in bed for the rest of the day. On the next day you can resume non-strenuous activity, but should refrain from intercourse for three to four days.
Post-Embryo Transfer Treatment
On the day of egg retrieval, you will receive an injection of progesterone. You should receive progesterone daily thereafter. The dose and form of progesterone will be decided at the time of transfer, and instructions given. In some cases, HCG is given instead of, or in addition to, progesterone. Fourteen days after embryo transfer, a blood pregnancy test (quantitative HCG) will be performed to determine if pregnancy has occurred. If it is positive, an ultrasound will be performed two weeks later to confirm pregnancy. If pregnancy progresses normally to 10-12 weeks, you will be referred to an Obstetrician for prenatal care.
Cancellation of a Cycle
About 10% of patients fail to respond to the fertility drugs. Some develop no follicles and some develop only a single follicle. These cycles are usually canceled as soon as this becomes apparent. Efforts are then made in subsequent cycles to find a regimen that results in sufficient follicular stimulation to proceed with the procedure. To maximize the chance of pregnancy, it is in your best interest that these procedures be done only after an optimal ovarian response.
Poor Gamete Performance in the Laboratory
In some cases, fertilization (union of sperm and egg) fails to occur. When this happens, we will look for reasons with both the sperm and egg that may be the cause of the failure. Certainly, if fertilization does not occur, there is no chance for pregnancy.
The Chances of Pregnancy
IVF is highly complex and technical. Many variables exist and there is no ideal stimulation protocol or average patient. It is for these reasons that each couple is evaluated thoroughly and treated with an individualized approach and treatment plan. The chances of achieving pregnancy, when everything is optimal, is no more than 35-50% per attempt.
View Pregnancy Success Rate Data
Caring for you, Caring for your heath & Caring for your future
5190 E Farness Drive #114 Tucson, Arizona 85712
(520) 326-0001